HOW BED SORES DEVELOP
You shift in your chair while sitting for prolonged periods, move your feet while standing , move many times during sleep. Every day we make many such subtle movements without being aware that we are doing it and thereby preventing pressure related problems. In fact if we do not change our positions often we start getting pain in that part.But for people immobilized by paralysis, injury or illness, those problems — including BED SORES — are a constant threat.
Importantly BED SORES do not always result from being in bed as the name implies.The location of the ‘BED SORES’ usuallydepends upon the position of the patient.
BED SORES can be caused by :
- Sustained pressure-When the skin and the underlying tissues are trapped two surfaces such as between bone and an external surface then the pressure prevents sufficient blood flow to supply the tissues with nutrients. The external surface may be a mattress, a chair or wheelchair, or even other parts of the body. The resulting bed sore represents the death of the involved soft tissue. This tends to happen in areas that aren’t well padded with muscle or fat and that lie just over a bone. For bed-bound patients, the sores are most likely to form on or around the lower back or tailbone – the commonest area in intensive care units -, the heels (especially in diabetics), & the hip-bone. Pressure ulcers(BED SORES) may also develop in a number of other areas, including the spine, ankles, knees, shoulders, and head, depending upon the position of the patient. Prolonged sitting may also contribute to formation of such ulcers especially in wheelchairs .
- Shear. – Sideways movement between two surfaces is shear. Your skin moves in one direction and the underlying bony and tendinous tissue moves in the opposite direction of movement. This happens when you slide down in a bed or chair. This force tears the capillaries and superficial skin layers and predisposes to the development of such wounds.
STAGES :
BED SORES occur in stages:
∙••••••••
Stage 1 ;begins as a persistent area of red skin that may itch or hurt and feel warm and spongy or firm to the touch.Stage I wounds are superficial and go away shortly after the pressure is relieved.
∙••••••••
Stage 2 – some skin loss has already occurred — either in the outermost layer of skin (the epidermis), the skin’s deeper layer (the dermis), or in both. The wound is now an open sore that looks like a blister or an abrasion, and the surrounding tissues may show red or purple discoloration.
∙••••••••
Stage 3 – has a crater-like ulcer extending deeper into the skin.
∙••••••••
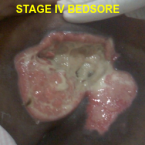
Stage 4 – This is the most serious and advanced stage. A large-scale loss of skin occurs, along with damage to underlying muscle, bone, and even supporting structures such as tendons and joints. There may also be a thick black scab(eschar ) present on the ulcer
STAGE IV BED SORE